Vagus Nerve
Anatomy
Welcome to our Vagus Nerve Anatomy guide!
This overview will provide insights into the route taken by the vagus nerve as it traverses the human body.
Join us as we follow the intricate pathways of this wonderous nerve. The medical images provided on this platform or within this content are intended for informational and educational purposes only. They are not a substitute for professional medical advice, diagnosis, or treatment.
Anatomical Structure of the Vagus Nerve
The Vagus Nerve, known as the tenth cranial nerve, is a remarkable anatomical structure characterized by its lengthy composition. It comprises both afferent (sensory, accounting for 80% of its fibers) and efferent (motor, making up 20%) fibers, giving it the appearance of a delicate, whitish vine or a flexible fiber optic cable. This intricate nerve network exhibits a somewhat lacy or feathery appearance, much like the intricate roots of a spreading tree, owing to its numerous branches and smaller nerve fibers. Afferent neurons, a crucial component of the vagus nerve, transmit sensory information from stimuli to the central nervous system and the brain, while efferent neurons carry neural signals away from the central nervous system to muscles, enabling movement and bodily function regulation.
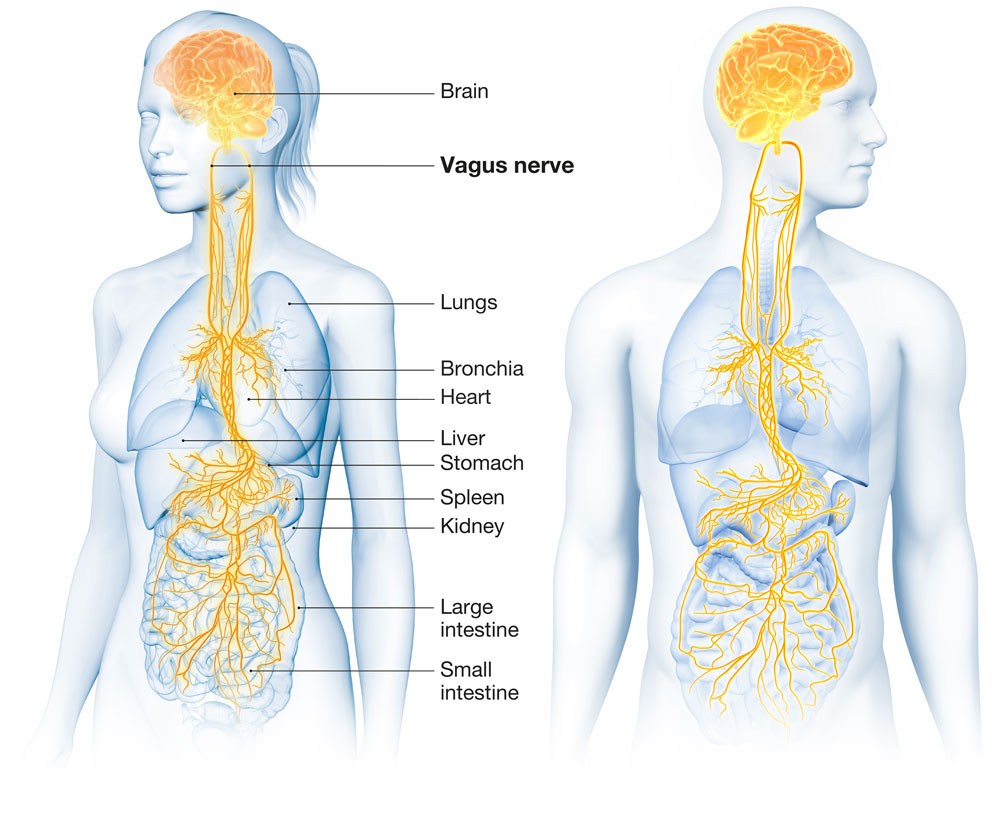
Did you know your vagus has its own signalling neurotransmitter and it's called Acetylcholine (ACh)?
The vagus nerve depends solely on ACh for communication with its assigned organs. This neurotransmitter is like the ultimate messenger in your central nervous system (CNS), ensuring signals get from point A to point B. Interestingly, it has different roles depending on which side of the CNS it's traveling on – whether it's the sympathetic or parasympathetic side, where the vagus nerve resides.
Now, let's discuss the production of ACh. It doesn't magically appear; rather, it undergoes a fascinating metabolic process. Acetylcholine is a combination of acetyl coenzyme A (acetyl-CoA) from your body's energy factories and importantly, choline from your diet. Choline takes a journey from your stomach through your bloodstream, with its destination being the nerve cells of the Vagus Nerve. Within the nerve cell, choline combines with Acetyl-CoA, facilitated by the enzyme Choline Acetyltransferase (ChAT), to create the neurotransmitter Acetylcholine.
So how do we get more of this amazing neurotransmitter. Boosting acetylcholine naturally involves a nutrient-rich diet with choline-rich foods, B-vitamins and omega-3 fatty acids. Antioxidant-rich foods, regular physical exercise, adequate sleep and stress management also contribute to a healthy supply of ACh. Consider acetylcholine precursors like choline supplements and explore herbal support with bacopa monnieri and huperzine A. Limit alcohol and caffeine intake and engage in brain-stimulating activities for overall cognitive health. Always consult a healthcare professional before adding supplements.
Another intriguing fact about Acetylcholine is that once it is created it doesn't just hang around idly. It's stored within nerve cells, ready to make its grand entrance to send signals to target organs. But here's the twist – after it's done its job, ACh doesn't stick around forever. Enter acetylcholinesterase (AChE), the cleanup crew. AChE breaks down Ach back into acetyl-CoA and choline, which isn't discarded but recycled. This recycled choline ensures a continuous supply of ACh, keeping the neural message flow smooth and uninterrupted.
So, the next time you're marvelling at the wonders of your smartphone, remember this: your brain and your vagus nerve have their very own direct messaging system called Acetylcholine, ensuring a seamless flow of signals through your vagus nerve to its target organs.

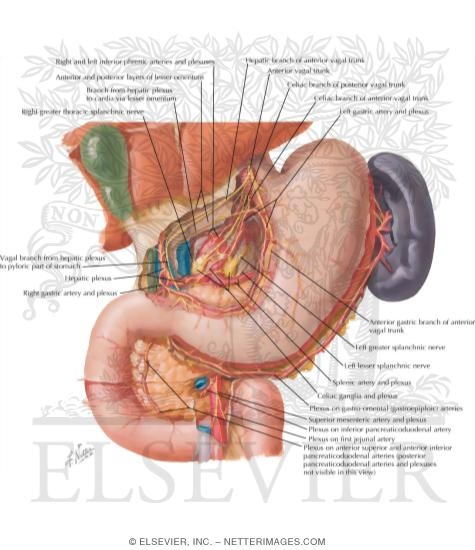
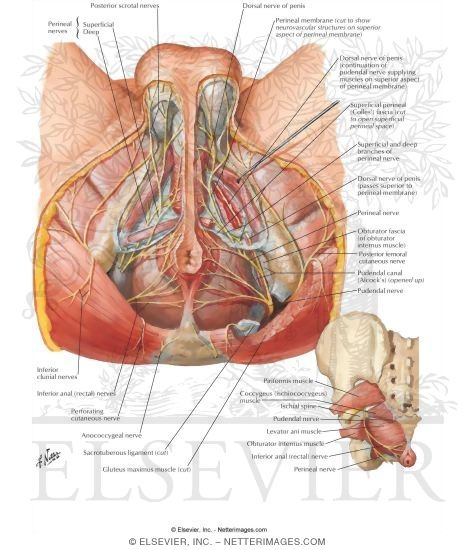
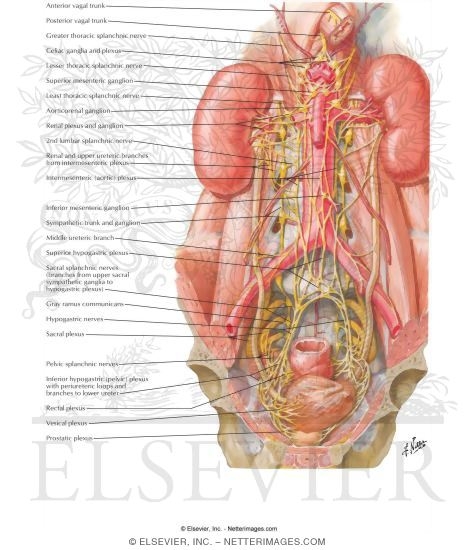
The Following are images that have been collated from The Netter Collection - one of the most comprehensive collection of hand-painted medical illustrations available with a 50+ year history and a brand identity recognised and accepted as the standard by anyone who has ever received some form of healthcare training.
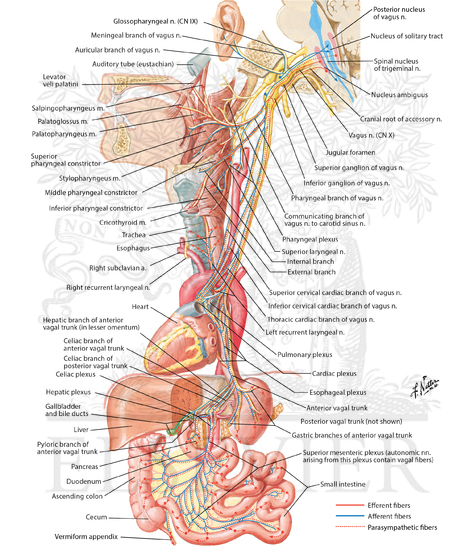
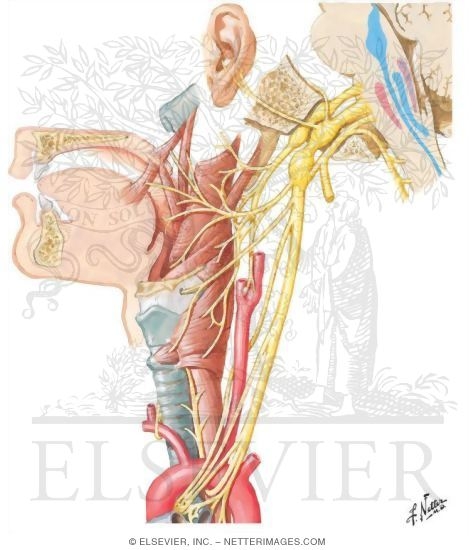
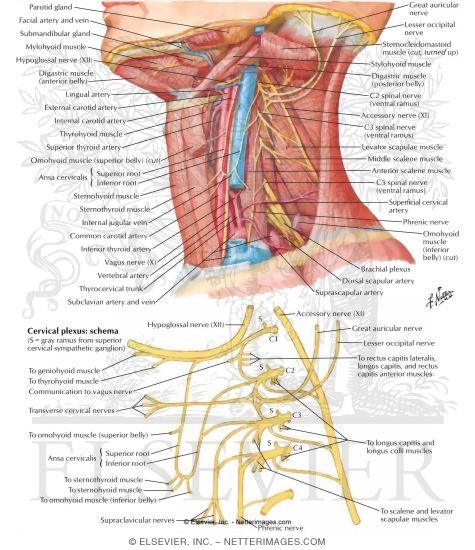
Illustration of Cervical Plexus In Situ Nerves of the Upper Extremity: Cervical Plexus from the Netter Collection
Learn more...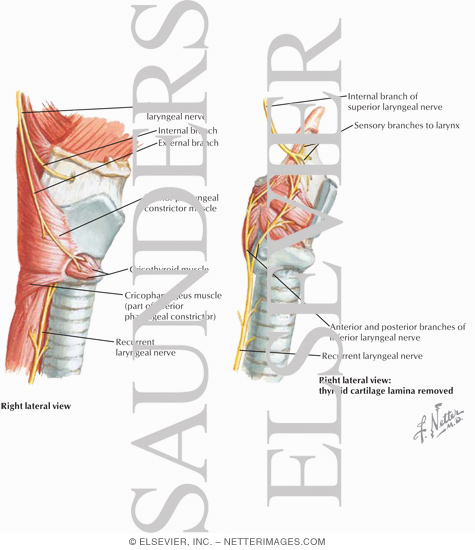
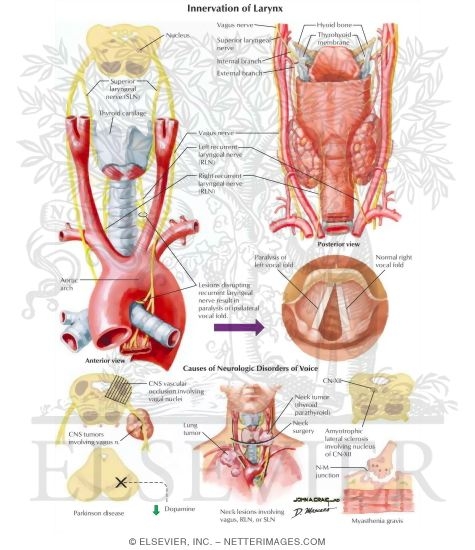
Illustration of Motor and Sensory Branches From the Vagus Nerve from the Netter Collection
Learn more...